Myofascial Release for Temporomandibular Joint (TMJ) Syndrome
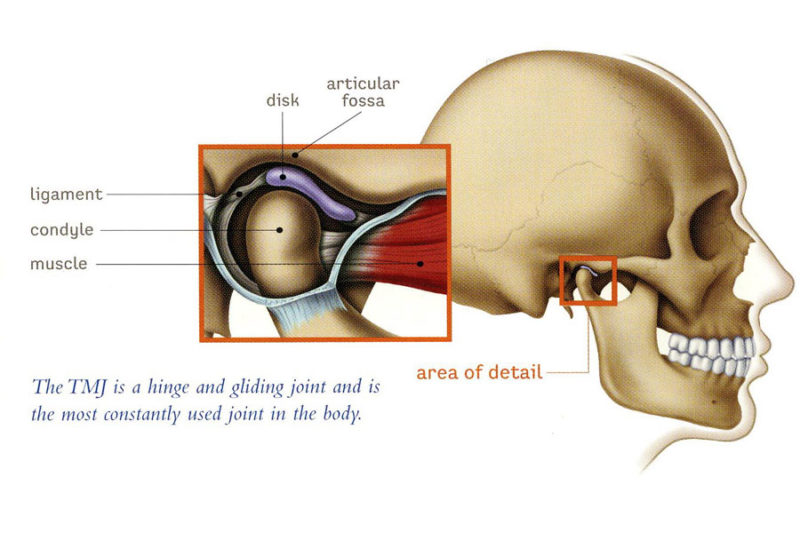
Temporomandibular Joint (TMJ) Syndrome is a term often used to describe temporomandibular disorders (TMD), which occur as a result of problems with the jaw, jaw joint, and surrounding facial muscles that control chewing and moving the jaw. The temporomandibular joint (TMJ) is the hinge joint that connects the lower jaw, or mandible, to the temporal bone of the skull. This bone is located immediately in front of the ear on each side of the head. When healthy, the joints are flexible, allowing the jaw to move smoothly up and down and side to side, also enabling a person to talk, chew, and yawn. Muscles attached to and surrounding the jaw joint control the position and movement of the jaw.
Myofascial Release (MFR) is a form of bodywork that eliminates pain, and restores motion and produces a profound healing effect on the body tissues. It has been proven to alleviate pain throughout the body, including pain resulting from temporomandibular joint syndrome.
What Happens at a Myofascial Release Treatment Session for TMJ?
In treating temporomandibular joint (TMJ) syndrome, the myofascial therapist will usually have confirmation of a diagnosis by a dentist. He or she will take a case history and further evaluate the fascial system. The therapist will observe the jaw movement, looking for range of motion (ROM) of the mandible. He or she will notice any differences in the outward appearance of the joint, and listen for popping or grating sounds during jaw movement. The therapist will also palpate (feel) the muscles of mastication (chewing) to get feedback on the patient’s pain or tenderness.
Myofascial treatment for temporomandibular joint (TMJ) disorders may involve the jaw, neck, mouth, and head. When the myofascial therapist has determined where the restrictions lie in the fascia, he or she will apply gentle pressure in the direction of the restriction, mobilizing the tissues to break up the viscosity of the ground substance found between two fascia layers.
Another technique is to release trigger points, or small contraction knots in the muscles that create referred pain to other areas of the body. Releasing trigger points will break into the chemical and neurological feedback loop that maintains the muscle contraction, increase circulation that has been restricted by the contracted tissue, and directly stretch the muscle fibers present.
Common trigger points of the jaw that cause temporomandibular joint (TMJ) syndrome can be found in the buccinator (a cheek muscle used for facial expressions, chewing, and tightening the cheeks for blowing); masseter (the major force for biting and chewing); and the pterygoid muscles, which are the key source of myofascial pain and temporomandibular disorder (TMD). By releasing the tension in these points, pain can be alleviated in the teeth, ear, eyes, head, and other areas of and around the jaw. This is done by holding sustained compression on trigger points, not just accessed on the outer surface of the face, but by working inside the mouth, as well.
In addition, those receiving treatment may receive education on lifestyle changes, such as eating soft foods, wearing a splint or night guard that fits over the upper and lower teeth, learning relaxation techniques, and avoiding extreme jaw movements. A muscle re-education exercise program may also be prescribed to improve alignment, focusing on specific areas of stretching and strengthening.
Is Myofascial Release Safe for TMJ Syndromes?
Although some physical discomfort may occur while the adhesions are released from deep in layers of fascia, myofascial release appears to be generally a safe therapy when performed by a properly trained practitioner. Practitioners are versed in avoiding areas of sensitivity and caution.
What is Myofascial Pain?
The “myo” in “myofascial” refers to muscle; “fascia” is the connective tissue covering muscles, organs, nerves, blood vessels, and bones throughout the body. Healthy fascia is flexible and wavy and is allowed to move without pain. Someone who has poor posture or has had physical trauma, repetitive stress injuries, scarring or inflammation might have more rigid fascia that does not move as easily. This damaged fascia can exert excessive pressure that produces pain or a decreased range of motion. It can also affect flexibility and stability. Often those who experience myofascial pain report seemingly unrelated symptoms. Compounding the issue is that myofascial restrictions do not show up in standard testing, so it has a good change of being misdiagnosed.
What Causes Temporomandibular Joint (TMJ) Disorders?
Asymmetry of the muscles of mastication (chewing), forward head posture, tightness of the back of the neck, and multiple Myofascial Trigger Points can cause TMJ problems. Injury to the jaw, temporomandibular joint (TMJ), or muscles of the head and neck—such as from a heavy blow or whiplash—can cause temporomandibular joint disorders (TMD). Also, grinding or clenching the teeth puts a lot of pressure on the TMJ. Additionally, the jaw is a ball-and-socket joint, and dislocation of the soft cushion or disk between the ball and socket can result in TMD. Those experiencing the wear and tear of osteoarthritis or the inflammation of rheumatoid arthritis in the TMJ can develop temporomandibular joint disorders. Finally, TMD can result from stress, which can cause a person to tighten facial and jaw muscles or clench the teeth.
What Are the Symptoms of Temporomandibular Joint (TMJ) Disorders?
There are several indicators that one is experiencing temporomandibular joint disorder (TMD). Common symptoms include:
- Pain/tenderness in the face, jaw joint area, neck and shoulders, and in or around the ear when chewing, speaking, or opening the mouth wide
- Limited ability to open the mouth very wide
- Jaws that get “stuck” or “locked” in the open- or closed-mouth position
- Clicking, popping, or grating sounds in the jaw joint when opening or closing the mouth (which may or may not be accompanied by pain)
- A tired feeling in the face
- Difficulty chewing or a sudden uncomfortable bite—as if the upper and lower teeth are not fitting together properly
- Swelling on the side of the face
Other common symptoms include toothaches, headaches, neck pain, dizziness, as well as earaches and hearing problems.